Patient Education Back to Patient Education
-
Abscessed Tooth
An abscessed tooth is an infected tooth. Your teeth contain tiny canals called root canals. Your root canals and the interior of your teeth contain pulp. Pulp is commonly infected by an untreated cavity. ... Read More
-
Adult Braces
More and more, braces are becoming very popular among adults. Adults realize the importance of a beautiful healthy smile and preventing future dental problems. There are a variety of braces to choose from; some are barely even noticeable. ... Read More
-
Apexification
Apexification is a treatment used to seal an open apex. The apex is the bottom part of a tooth’s root. Your teeth have tiny passageways called root canals. An open apex occurs when the root canals are not closed. ... Read More
-
Apicoectomy
An apicoectomy, also called a surgical root canal, is a dental treatment for an infected tooth root. An apicoectomy involves surgically removing the tip of the root and the infection. A filling is placed at the root tip.t ... Read More
-
Are braces uncomfortable?
It is common for most people to feel discomfort from braces from time to time. It may depend on the type of braces that you have and your age. Traditional braces may cause more discomfort than newer types of braces. ... Read More
-
Benefits of Braces
Orthodontics or “braces” can be helpful for both children and adults. They can straighten crooked teeth, correct the spacing between teeth, and improve bite patterns. Orthodontics can contribute to healthy teeth and gums and prevent future dental problems. ... Read More
-
Bisphosphonate and Osteonecrosis of the Jaw
Osteonecrosis of the jaw is a rare condition that can be caused by bisphosphonate medication. It is a serious disorder that causes severe bone destruction or loss. Osteonecrosis of the jaw may be treated with antibiotic rinses, removable mouth pieces. ... Read More
-
Bite Problems- Malocclusions
A malocclusion is a dental term for a bite problem. Everyone has some degree of malocclusion. However, significant malocclusions can contribute to mouth breathing and interfere with speaking and eating. A poor bite can cause teeth and enamel. ... Read More
-
Braces - Pediatrics
Orthodontics or “braces” are devices worn on the teeth to improve tooth alignment. Orthodontics can be helpful for both children and adults. Orthodontics can improve the function of your child’s teeth and the appearance of his or her smile. ... Read More
-
Braces and Tooth Care
Good oral health care is more important than ever once you have braces. Brushing and flossing removes food that can get caught in braces. Your orthodontist will provide you with an oral health care plan. Healthy habits ensure healthy teeth. ... Read More
-
Broken Braces (What to do)
Even though you may do everything to avoid it, it is common for braces to break at one time or another. Braces, brackets, bands, and wires may become loose or break because of chewing hard or sticky food. ... Read More
-
CariFree™ Cavity Prevention System
The CariFree™ system embraces advanced infection detection and treatment technology to prevent cavities before they start. In less than a minute, the CariFree™ system allows your dentist to measure the magnitude of harmful bacteria on your teeth. ... Read More
-
Cavities
Cavities are caused by tooth decay. Cavities are more common among children, but adults may develop them as well. Tooth decay occurs for several reasons including plaque formation, what you eat, the use of fluoride, how well you care etc. ... Read More
-
Cracked Teeth
Cracked teeth can result from grinding or clenching your teeth and chewing on hard objects, such as ice or hard candy. Cracked teeth may cause on again, off again pain and temperature sensitivity. You should contact your dentist soon. ... Read More
-
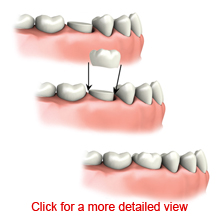
Crowns (Caps)
Introduction
A crown is a lab created “cap” that serves as a replacement for a tooth. It fits over a tooth or dental implant. Crowns restore a tooth’s strength, function, and appearance.
Essentially, a crown becomes the new outer layer for a tooth. Crowns are used for several reasons. Following root canal therapy, crowns are used to protect the remaining tooth and provide function. Crowns are used to cover a tooth with large fillings if the tooth structure has weakened. The teeth that are next to bridgework may be crowned to provide the bridge with a solid source of attachment. Additionally, a crown may be used with an implant to replace a lost tooth. A crown can also protect teeth with cracks and cover teeth that are discolored, chipped, or poorly shaped.
Crowns are created in a lab based on molds of your teeth and gums. Crowns are made of various materials depending on the strength requirement and desired appearance. Crowns can be made of porcelain, metal, such as gold, or a combination of both.
![Dr. Ernie Soto Dr. Ernie Soto]()
Symptoms
You may need a crown if you experience tooth fracture or loss. A crown is usually used in the final step of root canal therapy. A crown may be required if your tooth can no longer support a very large tooth filling. You may need crowns to support bridgework.Diagnosis
Your dentist can evaluate your need for a crown by examining your teeth and gums. Your dentist will check for loose, fractured, or decayed teeth. X-rays help identify changes in your teeth, bones, and gums.Treatment
Treatment with crowns usually requires two dental visits. First, impressions of your teeth are made to use as a mold for creating the new crown, and your tooth is prepared for crown placement. At your second visit, the new crown is secured in place.During your first appointment, your dentist will use molding material to create an impression of your teeth. A model of your teeth will be made from the impression. A lab technician will use your model as a guide when creating your custom made crown.Also during your first visit, your dentist will numb the area surrounding the affected tooth and prepare your tooth for the crown. A tooth typically needs to be made smaller to enable the crown to fit over it. After your tooth is prepared, your dentist will cover it with a transitional “temporary” crown to protect it until your permanent crown is placed.At your second appointment, the temporary crown is removed and the tooth is cleaned. Your dentist will evaluate the fit and appearance of the crown. Your dentist may adjust the crown to accommodate your bite pattern. Finally, your new crown is cemented in place.Your new crown can last for many years with proper care. It is important to brush your teeth at least twice daily and floss at least one time each day. Pay special attention to the areas surrounding your crown. Avoid grinding your teeth and chewing on hard items such as candy or ice. This can damage your crown. -
Dental Implants
Introduction
Dental implants are a beautiful natural-looking solution for missing teeth. They are the modern-day treatment of choice for tooth replacement. Dental implants are surgically placed in the jawbone. They serve as anchors for the attachment of replacement teeth, crowns, and partial or full dentures. Unlike dentures, there is no problem with slippage, so you can eat, speak, and smile with confidence. Overall, most people find that dental implants are comfortable, convenient, and improve the function and appearance of their teeth.
Dental implants may be an option if you are replacing a tooth or receiving a crown, partial dentures, or full dentures. Dental implants are not for everyone. Candidates for dental implants need to have healthy gums and bones to support the implant.
![Dr. Ernie Soto Dr. Ernie Soto]()
Diagnosis
Your dentist can evaluate if you are a candidate for dental implants by examining your teeth, gums, and jawbone. Your dentist will check for signs of gum disease and decay. X-rays and CT scans will be taken to determine the health of your teeth, gums, and the availability of bone.Treatment
Dental implant procedures require a series of appointments. It usually takes from three to nine months for the process to be completed. Dental implant surgery can take place in a dental office or a hospital as an outpatient procedure. You will receive a local pain reliever or be sedated for the surgery.
Surgery is required to place the dental implant in the jawbone. In some cases, a series of implants are joined together by a support bar. The bar provides security and stability for a full denture. After surgery, you will receive pain medication and antibiotics. You will initially need to eat a soft diet and refrain from strenuous activities.
It may take up to six months for your bone to fuse with the implant. After healing has taken place, your dentist will attach your crown or denture to the dental implant. This process may require several adjustments to achieve a good fit.
Your dental implants can last a lifetime with good oral health care. Our dentist will monitor your progress and design a maintenance program specifically for you. Make and attend all of your dental appointments. You should also brush and floss on a regular basis. Dental implant surgery is a highly successful procedure.
-
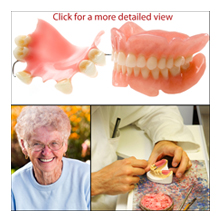
Dentures/Partial and Full
Introduction
Dentures are removable artificial teeth. Dentures can be partial or full. After tooth loss, dentures can restore your ability to eat and speak. They provide a natural looking smile while enhancing your facial appearance.Dentures are made of various materials to simulate the appearance of your natural teeth and gums. Your dentist will specifically match the color of your teeth and gums to that of your custom made dentures. Professionally made dentures are composed of premium long-lasting products, low-staining teeth, and high impact acrylic bases. With proper care, your dentures should last for a very long time.Dentures come in top and bottom pieces. You may wear upper, lower, or both upper and lower dentures. There are various types of dentures including conventional full dentures, intermediate full dentures, partial dentures, and overdentures.Conventional full dentures are appropriate for people that have lost all of their teeth on their upper or lower jaws. Conventional full dentures may be worn after your teeth have been extracted and your gums have healed. Healing can take several months. During the healing period, you are without teeth.Intermediate full dentures are another type of a complete denture. Intermediate dentures are worn after your teeth are removed and while your gums heal. This type of denture does not involve a period without teeth. Intermediate full dentures require dental visits before your tooth extraction to plan and fabricate the dentures. It may also require appointments after the initial fitting for adjustments to achieve an ideal fit.
Partial dentures are removable replacements for a series of extracted teeth. Partial dentures are held in place by attachments to adjacent natural teeth. The adjacent teeth are typically crowned to increase stability.
Overdentures are another denture option. Overdentures are removable artificial teeth that fit over existing natural teeth or implants. Overdentures are used to replace a small number of teeth. The underlying natural teeth are shaped to support and stabilize the overdenture.![Dr. Ernie Soto Dr. Ernie Soto]()
Symptoms
You may be a candidate for dentures if you have missing teeth. Many people need dentures after experiencing severe tooth decay and periodontal (gum) disease. Full dentures are used if you have lost all of your teeth. Partial dentures are used if you have remaining teeth.Diagnosis
Your dentist can evaluate if you are a candidate for dentures by examining your teeth, gums, and jawbone. Your dentist will check for signs of gum disease and decay. X-rays will be taken to determine the health of your teeth, gums, and bones.Treatment
The type of denture you receive is based on several factors, including your oral health, number of remaining teeth, and personal preferences. You will also need to determine the attachment method that you want. Your dentist will help you select the most appropriate options for you.People with good bone integrity may be candidates for dental implants. Dental implants are surgically placed metal anchors that attach to replacement teeth. They provide stability while preventing sliding. Dental implants are an option for full dentures, partial dentures, and overdentures.Partial dentures and overdentures are held in place with attachments to adjacent teeth. The attachments are usually made of metal. The adjacent teeth are frequently crowned to provide support and stability. Your natural teeth serve as a base from underneath the overdentures.Full dentures can be held in place without the aid of special attachments. The natural moisture in your mouth forms a vacuum to hold your dentures in place. If your dentures slip or slide, denture adhesive can help. If your dentures slip or slide too much, you should contact your dentist to have them adjusted.The amount of time it takes before you wear your new dentures depends on the type of dental procedures you need and the type of denture you select. The process typically takes a month, but some people may need more appointments than others. Expect a longer length of time if your gums need to heal after tooth extraction or if you receive dental implants.Dentures are created in the process of several dental appointments. The initial process involves making impressions of your teeth, gums, and jaws to fabricate a model to use for creating your dentures. Your dentist will have you bite on a piece of wax to record your bite pattern. Your dentist will determine the color of your teeth and gums. Your new dentures will match these colors to create a natural looking smile. When the initial process is completed, the molds, bite pattern, and color specifications are sent to dental lab that will custom make your dentures.Usually the dental lab will make a trial set before fabricating the final set of dentures. This allows your dentist an opportunity to check how the dentures fit and function in your mouth. The final dentures are made at the dental lab and sent to your dentist’s office.It may take you a while to get used to wearing your new dentures. You may need to practice eating and speaking. Let your dentist know if your dentures hurt, slip, or cause sores. Your dentist will gladly make adjustments.Initially, it may be easier for you to eat soft foods and foods that are cut into small pieces. Concentrate on chewing with both sides of your mouth. This puts even pressure on your dentures. Avoid eating chewy or sticky foods until after you get used to your new dentures.You should brush your gums and dentures daily to remove plaque. Use cool or warm water to avoid disfiguring the denture material. Dentures should be cleaned with a moistened soft denture brush or soft toothbrush. Ask your dentist to recommend a denture cleaning product. Denture cleaning paste is commonly used. Do not use toothpaste, bleach, or other household cleaning products. Prevent your dentures from drying out at night. When they are out of your mouth, soak your dentures in water or a denture cleanser.Take care when handling your dentures. They are fragile and can break. It is helpful to remove and insert your dentures while leaning over a folded towel placed on your vanity or a full sink of water. This can reduce the impact if you accidentally drop them.
Report any denture-related problems or discomfort to your dentist. Your dentist is happy to make denture adjustments quickly. It is common for dentures to need adjustments overtime because your jaw changes shape as you age. Some people may need to have more than one set of dentures made in their lifetime. Overall, dentures can last a very long time with good care. -
Diabetes and Oral Health
Introduction
Diabetes is a disease that affects how the body uses glucose, a sugar that is a source of fuel. Normally, insulin, a hormone, helps glucose enter the body cells where it is used for energy. There are different types of diabetes. People with Type 1 Diabetes do not produce insulin, and they must take insulin each day. People with Type 2 Diabetes produce insulin, but they either do not produce enough or the insulin does not work like it should. As a result, glucose does not get into the body cells.
People with diabetes need to check their blood glucose levels, alter their diets, exercise, and in some cases, take medications to maintain healthy blood glucose levels. Too much or too little glucose in the blood can make people ill and result in medical and dental complications. Uncontrolled diabetes can change the way that food tastes. It can promote dental-related infections and also slow the healing process of infections.
Dental problems can result from uncontrolled blood glucose levels associated with diabetes. Uncontrolled blood glucose levels impair white blood cells that are needed to fight infection. Infections can cause blood glucose levels to rise in people with diabetes. High glucose levels in saliva are fuel for the bacteria in your mouth. Bacteria in the mouth contribute to plaque and tartar build-up on your teeth and gums. This can cause tooth decay and periodontal (gum) disease. People with poor blood glucose control tend to develop periodontal disease more severely and more frequently than people with good control of their diabetes.
People with diabetes are more likely to develop mouth infections. People with diabetes that smoke, have high blood glucose levels, or take antibiotics have the highest risk for developing mouth infections. Some people develop dry mouth, a condition that causes a decrease in saliva production and contributes to infection. All of these factors can lead to fungal infections in the mouth such as oral candidiasis (thrush).
Symptoms
You should contact your dentist if you have the symptoms of a gum or mouth infection. Infections can make your gums bleed easily. You may notice this especially after you have just brushed or flossed your teeth. Your gums may look swollen or red. They may hurt or be tender when you touch them. Pus may develop on your gums. You may have bad breath or a bad taste in your mouth. Your teeth may separate or become loose. Loose teeth can cause your bite pattern to change. When you close your mouth to chew, your tooth alignment may feel different than it did before. Additionally, periodontal disease can change the way that your dentures fit.Diagnosis
Your dentist can diagnose dental problems associated with diabetes. You should tell your dentist that you have diabetes even if your blood glucose levels are controlled. Tell your dentist what your A1C level is and provide a list of medications that you take. Tell your dentist about your dental symptoms.Your dentist can diagnose periodontal disease and mouth infections by examining your teeth, gums, and soft structures in your mouth. Your dentist will check for loose teeth. Your dentist will gently insert a small periodontal probe between your teeth and gums to check for and measure gum detachment and pockets. X-rays help identify changes in your teeth, bones, or gums.Treatment
Your dentist can treat dental conditions related to diabetes. Candidiasis is treated by removing or controlling the causative factors. You should brush and floss your teeth according to your dentist’s instructions. Clean your dentures thoroughly. Do not wear dentures at night. If you have dry mouth, saliva substitutes can help.
Treatment for periodontal disease depends on the type of disease and how far it has spread. Initial treatments usually include a professional dental cleaning with scaling and root planning. Scaling is a procedure that removes plaque, tartar, and stains from the tooth surface. Root planning removes plaque and tartar while smoothing the root surface. The smooth surface makes it more difficult for plaque to attach to it. Root planning allows the gum tissues to heal next to the teeth.Some cases of periodontitis may require medications in addition to scaling and root planning. Your dentist may apply antibiotics to the site of infection. You may receive a prescription for antimicrobial mouth rinses to fight the bacteria that contribute to periodontitis. Advanced periodontitis may require tooth extraction and surgical treatment.After receiving professional treatment for periodontal disease or a mouth infection, good oral health care and blood glucose management can prevent the condition from recurring. Brush your teeth at least twice a day. Floss daily to remove plaque. Eat well-balanced meals, limit sugary or starchy foods, and avoid in between meal snacks.Make and attend regular dental appointments for professional cleaning and examinations. You should have your teeth examined and cleaned at least twice a year. Contact your dentist at the first sign of any diabetes-related dental problem. -
Dry Socket
Dry socket is a condition that can develop after a tooth is removed. Normally, a blot clot forms in the space where your tooth was at to protect the area while it heals. ... Read More
-
Eating Disorders and Tooth Care
Eating disorders are abnormal eating compulsions. People with eating disorders have a distorted body image. They attempt to control their weight by controlling their food intake. There are several types of eating disorders. ... Read More
-
Eating with Braces
There are a variety of orthodontic choices. Today’s braces range from clear aligners to clear or metal brackets. Some types of braces are removable, but non-removable braces make take a little time to get used to when eating. ... Read More
-
Endodontic Retreatment
Even with the best care, endodontic treatments occasionally need to be repeated. The most common repeated endodontic treatment is for an unsuccessful root canal that leads to endodontic infection. Initial treatments may fail for many reasons. Repeated endodontic treatments are used. ... Read More
-
Gum Disease and Periodontal Treatments
Introduction
Periodontal disease, commonly known as “gum disease,” is a leading cause of tooth loss in adults. It occurs when harmful bacteria infect the gums and create gaps around the teeth. Periodontal disease is termed a “silent disease” because it may not produce symptoms until it has progressed to an advanced stage. Periodontal disease is preventable, and your dentist can treat the condition. If left untreated, periodontal disease can lead to tooth, gum, and bone loss.
Your gums, periodontal ligaments, and underlying bones support your teeth and hold them in place. It is important to keep this foundation healthy. Your mouth contains bacteria. Some of the bacteria are good, and some types of bacteria can be harmful. A major cause of periodontal disease is bacteria that are found in plaque.
Plaque is a thin sticky film that constantly forms over your teeth. The sugar or starch in foods fuels plaque. The sugars mix with the bacteria in plaque to form destructive toxins. Plaque helps to hold the toxins in place against your teeth. Plaque that has hardened on your teeth is called tarter. Tarter provides plaque with an ideal growing space. Tartar can spread below your gums and onto your tooth’s root. This makes plaque removal very difficult.
Although periodontal disease is caused by plaque, several factors can increase the risk, severity, and pace of the condition. People who smoke or chew tobacco are more likely to develop periodontal disease. Structural problems, such as poor fitting dentures, poorly aligned teeth, and teeth grinding, can speed the progression of bone loss. Pregnancy and oral contraceptives (“the pill”) can exaggerate the gum’s response to plaque. Some medical conditions, such as HIV, AIDS, and diabetes, can lower resistance to infection and lead to more severe periodontal disease. Additionally, certain medications, including steroids, anti-epilepsy medications, chemotherapy, and some high blood pressure medications, can affect your gums.
Periodontitis is one of the most common types of gum disease. It is a progressive condition, meaning that it tends to get worse over time. However, periodontitis can be halted with early detection and treatment. This periodontal disease typically develops in stages: gingivitis, periodontitis, and advanced periodontitis.
Gingivitis is frequently, but not always, the first stage of periodontitis. Tartar on the roots of your teeth can lead to gingivitis. The plaque irritates your gums and causes them to pull away from your teeth, creating spaces or pockets. Gingivitis is a reversible disease if it is treated. Without treatment, gingivitis can lead to more serious conditions, including periodontitis and advanced periodontitis.
Periodontitis results from high levels of bacteria in plaque that release tissue-destroying enzymes. The enzymes damage the periodontal ligaments and bone that hold your teeth in place. Periodontitis creates bigger pockets around your teeth, which fill with and hold more damaging plaque. As the gums pull or recede further from your tooth, its roots become exposed. This can lead to tooth decay. The tooth decay can cause your teeth to be very sensitive to hot and cold temperatures. Treatments at this stage are aimed at stopping the disease and reversing its progression.
Periodontitis can progress to advanced periodontitis. At this stage the gums, supporting ligaments, and bones are damaged to an even greater extent. With such a weak foundation, tooth loss can occur. Although advanced periodontitis is not fully reversible with treatment, treatment can improve your oral health and prevent further destruction.
![Dr. Ernie Soto Dr. Ernie Soto]()
Symptoms
Periodontal disease can cause subtle symptoms at first. You may notice that your gums bleed when you brush or floss your teeth. Your gums may appear red and swollen. They may feel tender and recede from your teeth. You may experience bad breath and have a bad taste in your mouth. Call your dentist if you experience swollen gums, bleeding gums, or loose teeth.As the disease progresses, you may notice deep pockets forming between your teeth and gums. Your teeth may feel lose or shift easily. When you chew, your teeth may feel like they are out of alignment or in different positions than they were before. Pain usually does not occur until advanced periodontal disease.Diagnosis
Your dentist can diagnose periodontal disease by examining your teeth and gums. Your dentist will gently insert a small periodontal probe between your teeth and gums to check for and measure gum detachment and pockets. Your dentist will check for loose teeth. X-rays help identify changes in your teeth, bones, or gums.Treatment
Treatment for periodontal disease depends on the type of disease and how far it has spread. Initial treatments usually include a professional dental cleaning with scaling and root planning. Scaling is a procedure that removes plaque, tartar, and stains from the tooth surface. Root planning removes plaque and tarter while smoothing the root surface. The smooth surface makes it more difficult for plaque to attach to it. Root planning allows the gum tissues to heal next to the teeth.
Some cases of periodontitis may require medications in addition to scaling and root planning. Your dentist may apply antibiotics to the site of infection. You may receive a prescription for antimicrobial mouth rinses to fight the bacteria that contribute to periodontitis.
Advanced periodontitis may require tooth extraction and surgical treatment. Surgery can involve the gums and bones. A gingivectomy is a procedure that removes the pocket wall in the gums to allow the tooth to be cleaned and prevent infection. It is not a common procedure. Flap surgery is a more common treatment for deep gum pockets. This procedure temporarily removes the gums from the teeth to allow the removal of plaque, tarter, and diseased tissue. The gum tissue is then stitched into the best position to ensure easy cleaning.
Osseous surgery is a type of bone surgery that may be performed at the same time as flap surgery. Osseous surgery is a procedure to remove or reshape damaged bone surrounding a tooth. In some cases, a bone graft may be used to replace bone loss and stabilize a tooth. Following osseous surgery, splints similar to braces are applied to temporarily provide stability while healing takes place.
After receiving professional treatment for periodontal disease, good oral health care can prevent the condition from recurring. Brush your teeth at least twice a day. Floss daily to remove plaque. Eat well-balanced meals, limit sugary or starchy foods, and avoid in between meal snacks. Finally, make and attend regular dental appointments for professional cleaning and examinations.
-
Invisalign
Invisalign® is the newest product in tooth straightening systems. Unlike traditional metal braces, Invisalign® Aligners are clear and nearly undetectable. They are conveniently removable for eating, brushing, and flossing your teeth. Invisalign® Aligners are comfortable. ... Read More
-
Jawbone Grafts
Jawbone grafts are a modern dental technique used to reconstruct damaged areas of bone. Jawbone grafts may be necessary if gum disease, trauma, or medical conditions have caused your jawbone to deteriorate. Bone grafts enable dental implant surgery and prosthetics . ... Read More
-
Kids: What's it Like to Wear Braces?
You may already know other kids that have braces, like your classmates or brothers and sisters. You may have seen old photos of your parents wearing braces and now it’s your turn and you’re wondering, “What’s it like to wear? ... Read More
-
Methamphetamine and Oral Health
Methamphetamine is an illegal street drug. It is a stimulant that produces a prolonged high or euphoric state. Methamphetamine use is a threat to your child’s general health and oral health. . ... Read More
-
Mouth Piercings and Jewelry
Mouth piercings and jewelry are a type of fashion trend among some young adults and teenagers. The lips, tongue, and cheeks may be pierced to wear barbell, hoop, or stud-type jewelry, similar to earrings. Oral piercing procedures and the jewelry. ... Read More
-
Mouth Sores
Mouth sores are a common condition. They can cause pain and discomfort. Some develop inside of the mouth and others develop on the lips and skin surrounding the mouth. There are several different types of mouth sores. ... Read More
-
Oral Cancer
Introduction
Oral cancer can occur on the lips, tongue, gums, or other tissues inside of the mouth. It most commonly occurs on the lower lip. Oral cancer is more common in people over the age of 40 years old. It occurs more frequently in men than in women. People who smoke cigarettes, pipes, or cigars or chew tobacco have the highest risk for oral cancer. People that use tobacco and heavily consume alcohol have even a greater risk.
Signs of oral cancer include a sore or irritation that does not heal or go away. Early oral cancer may not cause pain and may not be noticed. You can reduce your chances of developing oral cancer by avoiding tobacco and alcohol products. Oral cancer has a fair prognosis. It is treated with surgery, radiation therapy, and chemotherapy.
Symptoms
You may or may not notice the early signs of oral cancer. It usually does not cause pain in the early stages. Oral cancer may begin as a white or red patch on your gums, tongue, inside of your cheek, or inside or outside of your lips. It may look like a sore or irritation that does not heal or go away. The affected area may bleed easily. Oral cancer can also begin as a lump, thick area, or crusty area. It can cause part of your mouth to feel numb.You may experience difficulty swallowing food or moving your tongue. It may feel like something is caught in your throat. Your voice may change or sound hoarse. Your bite pattern may change. You may have difficulty bringing your jaws together or chewing food. Swelling may cause your dentures to not fit properly.Diagnosis
Your dentist or doctor can diagnose oral cancer by reviewing your medical history, examining your mouth, and taking some tests. You should tell your doctor about your risk factors and symptoms. A small bit of tissue from a suspected area may be taken for examination in a laboratory.Treatment
You may be referred to a specialist for treatment of oral cancer. The type of treatment you receive depends on the location and extent of your cancer. Oral cancer that has spread to other parts of the body (metastasized) will need treatment also. Oral cancer is treated with surgery, radiation therapy, chemotherapy, or a combination of treatments. Cosmetic surgery can help to maintain your facial appearance after surgery. -
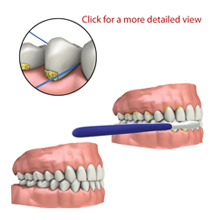
Oral Health
Introduction
Good oral health care includes professional dental treatments provided by your dentist and good habits at home. You should eat well-balanced meals and limit between-meal snacks. Keep your teeth clean by brushing and flossing. Healthy habits ensure healthy teeth and gums by preventing tooth decay and gum disease.
Your gums, periodontal ligaments, and underlying bones support your teeth and hold them in place. It is important to keep both this foundation and your teeth healthy. Your mouth contains bacteria. Some of the bacteria are good, and some types can be harmful to your teeth. Bacteria contained in plaque are a major cause of tooth decay and gum disease.
Plaque is a thin sticky film that constantly forms over your teeth. The sugar or starch in foods fuels plaque. The sugars mix with the bacteria in plaque to form destructive toxins.Plaque helps to hold the toxins in place against your teeth. Plaque plays a major role in tooth decay. Plaque that has hardened on your teeth is called tarter. Tartar provides plaque with an ideal growing space. Plaque and tartar build up can lead to gum disease.
![Dr. Ernie Soto Dr. Ernie Soto]()
Symptoms
Plaque is constantly forming on your teeth. It may cause your teeth to not “feel clean.” Additionally, pieces of food may stick to your teeth or get caught in between your teeth when you eat.Diagnosis
Your dentist can recommend an oral heath care plan for you at your dental examination. Your dentist will examine your teeth and gums. Your dentist can prescribe mouth rinses and fluoride treatments if you need additional care.Treatment
Home treatment involves regular brushing and flossing. You should brush your teeth twice daily. Floss your teeth once a day. You should follow the specific instructions provided by your dentist.Brush your teeth with a toothpaste containing fluoride. Your dentist may recommend special types of toothpaste for you. In some cases, dentists prescribe prescription toothpaste containing larger amounts of fluoride or plaque fighting ingredients.Your dentist can recommend the type of toothbrush that is most appropriate for you. Toothbrushes come in a variety of sizes and bristle types. To begin brushing your teeth, hold your toothbrush at a 45° angle and place it against your gums. Gently move the toothbrush in circular strokes. Brush all sides of your teeth’s surfaces. Use up and down strokes to brush the front of your teeth. In addition to brushing your teeth, make sure you brush the soft surfaces in your mouth including your gums and tongue.There are a variety of dental flosses to choose from. Your dentist can recommend the most appropriate one for you. To floss your teeth, first break off about 18 inches of dental floss and wrap the ends of the floss around the middle fingers on both of your hands. Use your thumbs and index fingers to maneuver the floss in your mouth.Place the floss gently between your teeth. Gently move the floss in the space between your tooth and gum. Move the floss against the side of your tooth while moving it away from your gum. You should floss between each of your teeth and the back side of your last tooth.Good oral health helps to ensure healthy teeth and a lasting smile. Practice good habits at home. Make and keep all of your dental appointments. -
Orthodontic Phasing
In the past, orthodontics were mainly for teenagers. More and more, adults are wearing braces as well. Orthodontists recognize the importance of healthy teeth and gums across the life span. Today, early proactive treatment delivered in phases during early childhood. ... Read More
-
Orthodontics
Orthodontics or “braces” are devices worn on the teeth to improve tooth alignment. Orthodontics can be helpful for both children and adults. Orthodontics can improve the function of your teeth and the appearance of your smile. ... Read More
-
Pain Free Dentistry
Your comfort and safety are among your dentist’s top concerns. There are several options for pain-free dentistry. Your dentist is happy to discuss and use the most appropriate method for you. Knowing that your visit will be pain-free can help. ... Read More
-
Pediatric Traumatic Dental Injuries
Pediatric dental emergencies include broken, chipped, or injured loose teeth. Pediatric dental emergencies are conditions that cause your child pain or threaten the health of your child's teeth and gums. It also includes cracked teeth, bleeding gums, and fillings that have come out. ... Read More
-
Pediatrics - Mouth Piercings and Jewelry
Mouth piercings and jewelry are a type of fashion trend among some young adults and teenagers. The lips, tongue, and cheeks may be pierced to wear barbell, hoop, or stud type jewelry, similar to earrings. ... Read More
-
Pediatrics - Mouthguards for Sports
Mouthguards are protective coverings worn over the teeth. They provide protection to a child’s mouth, teeth, tongue, and gums during contact or impact sports. There are several types of mouthguards. Your dentist can help you choose the most appropriate one. ... Read More
-
Pediatrics - Teething
Babies may start getting teeth their first teeth at as early as six months old. Some babies may experience discomfort as the teeth begin to come in and break through the gum. Babies respond to teething and teething treatments differently. ... Read More
-
Pediatrics - Thumb Sucking
Thumb sucking is a natural reflex for babies. They may suck on their thumb, pacifier, or other objects to relax, induce sleep, explore their world, or for security. Youngsters usually stop thumb sucking between the ages of two and four. ... Read More
-
Retainers
Retainers are orthodontic devices that are worn after braces are removed. The purpose of retainers is to keep your teeth in alignment following orthodontic treatment. Retainers can be removable or permanent and custom-made to fit your mouth. ... Read More
-
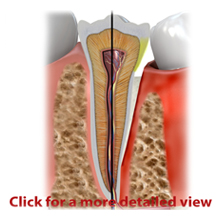
Root Canal
Root canal therapy or “root canal” is a procedure to treat and save damaged and infected teeth. Before root canal therapy, the only treatment for affected teeth was removal. Today, root canal therapy is a common procedure. ... Read More
-
Sedation Dentistry
Introduction
It is very common for people to have fear or feel nervous about visiting their dentist. Sedation dentistry is helpful for people that experience high levels of anxiety during dental procedures. Sedation dentistry makes you feel very relaxed during your visit. It is also used for longer procedures, including dental surgery and wisdom tooth extraction. Your dentist can provide “conscious sedation” or general anesthesia.
Conscious sedation uses medications that allow you to be very relaxed, yet awake and responsive. General anesthesia medications create a deep sleep-like state. Sedative medications are frequently used with pain-relieving medications.
Symptoms
It is very common for some people to have a general fear of going to the dentist. Others may have anxiety disorders that are heightened during a dental visit. Your dentist is happy to discuss your concerns and select options that are appropriate for you.Sedation dentistry makes you feel very relaxed during the procedure. It is especially helpful if you have anxiety. Sedation dentistry is also used for people with physical disabilities that have uncontrollable movement disorders.Diagnosis
Tell your dentist if you or your child experiences fear and anxiety before and during dental visits. Tell your dentist if you have an anxiety disorder. It is important to tell your dentist what medications you take and what other medical conditions you have. Inform your doctor of your drug allergies.
It is very important to tell your doctor if you consume alcohol or use illegal street drugs. It is also very important to tell your doctor if you have experienced a neurological disorder, such as a traumatic brain injury or a stroke. Your doctor needs to consider all of this information when selecting and dosing the appropriate medication for you.
Treatment
You can receive anti-anxiety or sedative medications before or during your visit. You will need to have someone else drive you to and from your dentist’s office. Anti-anxiety or sedative medications are administered as pills, liquids, gases, or injections. They can be used in conjunction with pain-relieving medications.Conscious sedation methods use nitrous oxide, commonly referred to as “laughing gas.” You can receive nitrous oxide by inhaling it through a small mask or having it administered intravenously (IV sedation). Nitrous oxide causes you to feel very relaxed and less aware of your surroundings. You remain awake and are responsive during the procedure. Your dentist must have a state permit to administer conscious sedation.General anesthesia produces a deep sleep and loss of consciousness. It makes you temporarily not alert, not aware of your surroundings, and not able to respond. You are monitored during this time. The medication wears off shortly after the procedure, and you become alert again. General anesthesia is very useful for people with uncontrollable anxiety or uncontrollable body movements from neurological disorders. Your dentist must have a state permit to administer general anesthesia.Your comfort and safety are top concerns of your dentist during your visit. Ask your dentist if sedative dentistry is an option for you. Knowing what to expect at your visit can help you relax and ease your fear about dental procedures.
-
Sensitive Teeth
Sensitive teeth are a very common condition. Sensitive teeth cause brief pain or discomfort when the teeth come in contact with hot or cold temperatures from the air, food, or beverages. Cavities, cracked teeth, eroded teeth, and gum disease. ... Read More
-
Space Maintainers
Space maintainers are small appliances that are worn to maintain a space between teeth. A space maintainer may be necessary if a “baby tooth” or primary tooth is lost before the permanent replacement tooth is ready to come in. ... Read More
-
Teeth Grinding (Bruxism)
Teeth grinding, called bruxism, results from repeatedly clenching and releasing the jaw muscles. Both children and adults can experience bruxism. It may occur during the day or night. It is caused by several factors including stress, certain medications, certain illegal. ... Read More
-
Teeth Whitening- External Stains
Teeth whitening can lighten the shade of your teeth and brighten the appearance of your smile. Teeth whitening systems remove or bleach external stains on your teeth. Your teeth can become stained, darker, or discolored over time. ... Read More
-
TMJ- Temporomandibular Joint Disorder
Temporomandibular Joint Disorder (TMJ) is a condition that affects the jaw joint. Your lower jaw attaches to your skull by muscles and the two temporomandibular joints located near your ears. Your jaw opens, closes, and moves from side to side. ... Read More
-
Tooth Anatomy: An Overview of Your Teeth
Your teeth serve many purposes. They help you chew food. Teeth work with your tongue to help you form sounds to speak. Teeth also create your beautiful smile and give your face its shape. Teeth vary in shape, size, location. ... Read More
-
Tooth Extraction
Tooth extraction may be necessary for several reasons. Teeth may need to be removed if they are decayed or infected. In some cases, teeth are removed prior to orthodontic procedures. Wisdom teeth are commonly extracted. ... Read More
-
Tooth Fillings
Tooth fillings are substances used to restore teeth following tooth decay or injury. They prolong the life of your natural teeth. Fillings fill in openings on a tooth after a cavity is removed or a crack has occurred. ... Read More
-
Veneers
Veneers are thin artificial coverings that are applied over the front of your natural teeth. Veneers are used to correct the appearance of chipped, cracked, or gapped teeth and tooth discoloration. There is more than one type of veneer. ... Read More
-
Wisdom Teeth
Wisdom teeth are the third and final set of molars. Some people may not develop a full set of wisdom teeth. Others may not develop any at all. It is very common for wisdom teeth to require dental treatment. ... Read More
-
Your General Examination Visit- What to Expect
A general dental examination and tooth cleaning can help you achieve and maintain excellent oral health. It is important to receive preventative care and have your dentist treat any problems as soon as they arise. ... Read More
-
ZOOM!® - Teeth Whitening
The Zoom!® Professional Whitening System (Zoom!®) is one of the newest ways to whiten your teeth and brighten your smile. Zoom!® is a bleaching process that safely lightens discolored teeth. It is quick and easy. ... Read More

Copyright © 2022 - iHealthSpot Interactive - www.iHealthSpot.com
This information is intended for educational and informational purposes only. It should not be used in place of an individual consultation or examination or replace the advice of your health care professional and should not be relied upon to determine diagnosis or course of treatment.
The iHealthSpotpatient education library was written collaboratively by the iHealthSpot editorial team which includes Senior Medical Authors Dr. Mary Car-Blanchard, OTD/OTR/L and Valerie K. Clark, and the following editorial advisors: Steve Meadows, MD, Ernie F. Soto, DDS, Ronald J. Glatzer, MD, Jonathan Rosenberg, MD, Christopher M. Nolte, MD, David Applebaum, MD, Jonathan M. Tarrash, MD, and Paula Soto, RN/BSN. This content complies with the HONcode standard for trustworthy health information. The library commenced development on September 1, 2005 with the latest update/addition on February 16, 2022. For information on iHealthSpot’s other services including medical website design, visit www.iHealthSpot.com.
Office Hours
MON - THU9:00 am - 5:00 pm
FRI9:00 am - 1:00 pm
SAT - SUNClosed
Address: 10187 Cleary Blvd STE 103, Plantation, FL 33324
Email: [email protected]
Phone: (954) 368-6264